What is endometriosis?
Endometriosis occurs when the tissue that lines the womb (the endometrium) grows outside the womb – usually in the pelvic cavity behind the womb or on the ovaries.
How do I know if I have endometriosis?
The most common symptom of endometriosis is painful periods. Quite often women with endometriosis have experienced pain from their first period or when they were at school. Every person experiences pain differently and other pain symptoms can include heavy periods, spotting before a period, pain with intercourse, bladder pain, bowel pain, stabbing abdominal pain, headaches, nausea and fatigue. Women with painful periods have on average 8 of these symptoms and it can be difficult to know if endometriosis is the cause of them or another condition that causes pelvic pain. We wrote a paper about the symptoms that women with period pain experience, VIEW IT HERE.
How is endometriosis diagnosed?
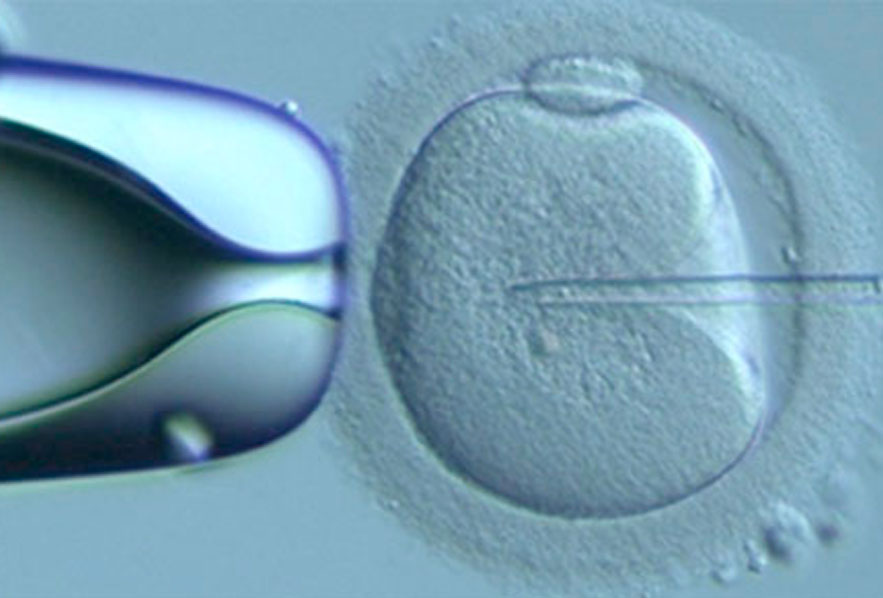
The only way that you can be sure that you have endometriosis is to look for endometrial tissue in the pelvis, using a small telescope( laparoscope)that is inserted through the belly button while you are asleep during a surgical procedure.
A small number of ultrasound specialists can perform scans that specifically look for endometriosis which are accurate about 60% of the time. MRI (magnetic resonance imaging) endometriosis specialists can also sometimes see features that suggest endometriosis.
Some women do have endometriosis even through it isn’t seen on ultrasound or MRI and laparoscopic surgery is the only way of knowing for sure if you have endometriosis. We have reviewed how well the imaging tests detect endometriosis in THIS REPORT.
Why does endometriosis make it more difficult become pregnant?
The (endometrium) lining of the womb grows then breaks down in response to the cyclical changes in reproductive hormones. When the tissue breaks down it leaves the body as a period.
When the endometrial tissue is in the pelvic cavity (endometriosis) the tissue breaks down but it can’t leave the body and it becomes trapped. Signals from dying cells in the tissue attract immune cells which try to clear the tissue. This process creates an inflammatory environment and high levels of cellular stress as well as swelling and pain in the pelvic cavity. Eggs sperm and embryos have a much tougher job to stay healthy in this inflammatory environment and it is harder for them to create a pregnancy. Women with endometriosis can still conceive naturally but it may take longer and if other factors (like a mild reduction in sperm quality) are present it can be even more difficult.
What fertility treatments are available for endometriosis?
Improving the environment that egg, sperm and embryos are in helps fertility. A healthy lifestyle, good diet, avoiding smoking, too much coffee or alcohol and managing pain will help. Taking pregnancy multivitamins are also beneficial.
Flushing the fallopian tubes with a fluid called lipiodol has been shown in a large Dutch study to improve the chance of natural conception and the higher pregnancy rates were particularly apparent in the group of women that had endometriosis. Lipiodol didn’t change pregnancy rates if women with endometriosis were having IVF.
Surgery provides a diagnosis and if the lesions are removed can improve the environment for eggs sperm and embryos. Couples have a better chance of conceiving in the 6 months after surgery. Of those who want a baby, 50% will conceive after surgery, 2/3rds naturally and 1/3 using IVF.
IVF is another option as the eggs sperm and embryos are removed from the pelvic environment and cultured in the lab. Women with endometriosis have fewer eggs retrieved at an IVF egg pickup, less embryos fertilise and there are fewer embryos than other women having IVF. But usually there are a small number of good embryos and only one is needed to create a pregnancy. This means that although there may be less numbers of embryos to choose from, if the one that transferred into the womb, if good quality it is just as likely to create a pregnancy as embryos from other couples. For this reason, the pregnancy rates for women with endometriosis having IVF are similar to those of other women with different fertility problems.
Why are the eggs numbers lower for women with endometriosis?
Women with endometriosis have a tendency to lower egg numbers, which is likely to be because it is harder for the eggs to survive in an inflammatory environment. Surgery, particularly operations that involve operating on endometriosis cysts on the ovaries (endometrioma’s) can also lower egg numbers. For this reason American, British and Australian guidelines recommend that the decision about whether to do surgery or have IVF treatment to improve fertility, is carefully considered for each couple taking into account factors like age, the egg numbers in the ovary, pain symptoms and the time trying to conceive. Any surgery should be performed by highly qualified endometriosis surgeons and as few as possible surgeries should be undertaken.
If women with endometriosis have low egg numbers they can consider freezing their eggs. This is not a perfect technology and each egg has only about a 7% chance of creating a pregnancy (and there is no guarantee). Usually we try to freeze and store 15-20 eggs if possible.

Is it more difficult for the lining of the womb to accept an embryo if I have endometriosis?
This is controversial. Some researchers have found that the lining of the womb is less responsive to the hormone progesterone (which keeps the lining of the womb stable and helps implantation and placental development). This may be why some women with endometriosis get spotting in the week leading up to their period and why we sometimes prescribe progesterone in the second half of a conception cycle. There is good evidence in fresh and frozen embryo transfer cycles where additional hormones are given, the quality of the embryo mainly determines if a pregnancy will result and not the responsiveness of the lining of the womb.
What should I do if I think I have endometriosis and want to conceive?
The first step is to talk to you doctor explaining your concerns and to say that you think you might have endometriosis. They are likely to recommend seeing a gynaecologist or fertility specialist with a particular interest in treating endometriosis. Specialised ultrasound or MRI scans may be considered, your ovarian reserve may be estimated with a blood test. Your doctor should provide all the options for treatment and the costs and likely success of these treatments and provide all the information and advice you need to make a treatment decision. Managing pain may also be an important part of your fertility treatment plan and can influence decisions about when to consider surgery and when is right time to explore IVF and other treatment options.

Many couples who have endometriosis as a factor in their fertility journey do conceive naturally and still more conceive using IVF and other fertility treatments. Getting good advice about your reproductive health, and being well informed of your options, gives you the ability to make the best decisions based on your individual set of circumstances.